What exactly is a thyristor?
A thyristor is actually a high-power semiconductor device, also referred to as a silicon-controlled rectifier. Its structure consists of 4 quantities of semiconductor elements, including three PN junctions corresponding towards the Anode, Cathode, and control electrode Gate. These three poles are the critical parts from the thyristor, allowing it to control current and perform high-frequency switching operations. Thyristors can operate under high voltage and high current conditions, and external signals can maintain their working status. Therefore, thyristors are widely used in a variety of electronic circuits, such as controllable rectification, AC voltage regulation, contactless electronic switches, inverters, and frequency conversion.
The graphical symbol of any semiconductor device is usually represented by the text symbol “V” or “VT” (in older standards, the letters “SCR”). Additionally, derivatives of thyristors include fast thyristors, bidirectional thyristors, reverse conduction thyristors, and light-controlled thyristors. The working condition from the thyristor is the fact that whenever a forward voltage is used, the gate will need to have a trigger current.
Characteristics of thyristor
- Forward blocking
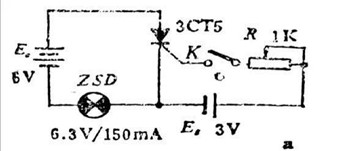
As shown in Figure a above, when an ahead voltage can be used involving the anode and cathode (the anode is attached to the favorable pole from the power supply, as well as the cathode is attached to the negative pole from the power supply). But no forward voltage is used towards the control pole (i.e., K is disconnected), as well as the indicator light does not illuminate. This demonstrates that the thyristor is not conducting and contains forward blocking capability.
- Controllable conduction
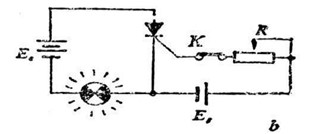
As shown in Figure b above, when K is closed, along with a forward voltage is used towards the control electrode (known as a trigger, as well as the applied voltage is referred to as trigger voltage), the indicator light turns on. This means that the transistor can control conduction.
- Continuous conduction
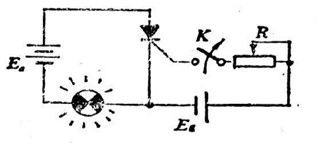
As shown in Figure c above, right after the thyristor is excited, whether or not the voltage in the control electrode is removed (that is, K is excited again), the indicator light still glows. This demonstrates that the thyristor can still conduct. At this time, in order to cut off the conductive thyristor, the power supply Ea should be cut off or reversed.
- Reverse blocking
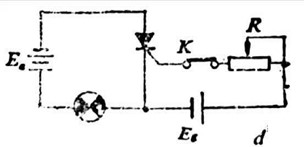
As shown in Figure d above, although a forward voltage is used towards the control electrode, a reverse voltage is used involving the anode and cathode, as well as the indicator light does not illuminate currently. This demonstrates that the thyristor is not conducting and can reverse blocking.
- In summary
1) If the thyristor is subjected to a reverse anode voltage, the thyristor is in a reverse blocking state no matter what voltage the gate is subjected to.
2) If the thyristor is subjected to a forward anode voltage, the thyristor will only conduct once the gate is subjected to a forward voltage. At this time, the thyristor is within the forward conduction state, which is the thyristor characteristic, that is, the controllable characteristic.
3) If the thyristor is excited, provided that there exists a specific forward anode voltage, the thyristor will always be excited regardless of the gate voltage. That is, right after the thyristor is excited, the gate will lose its function. The gate only serves as a trigger.
4) If the thyristor is on, as well as the primary circuit voltage (or current) decreases to close to zero, the thyristor turns off.
5) The problem for your thyristor to conduct is the fact that a forward voltage needs to be applied involving the anode as well as the cathode, as well as an appropriate forward voltage also need to be applied involving the gate as well as the cathode. To transform off a conducting thyristor, the forward voltage involving the anode and cathode should be cut off, or even the voltage should be reversed.
Working principle of thyristor
A thyristor is essentially a distinctive triode composed of three PN junctions. It may be equivalently thought to be comprising a PNP transistor (BG2) as well as an NPN transistor (BG1).
- In case a forward voltage is used involving the anode and cathode from the thyristor without applying a forward voltage towards the control electrode, although both BG1 and BG2 have forward voltage applied, the thyristor remains switched off because BG1 has no base current. In case a forward voltage is used towards the control electrode currently, BG1 is triggered to create basics current Ig. BG1 amplifies this current, along with a ß1Ig current is obtained in its collector. This current is precisely the base current of BG2. After amplification by BG2, a ß1ß2Ig current is going to be brought in the collector of BG2. This current is sent to BG1 for amplification and after that sent to BG2 for amplification again. Such repeated amplification forms an essential positive feedback, causing both BG1 and BG2 to get into a saturated conduction state quickly. A large current appears inside the emitters of the two transistors, that is, the anode and cathode from the thyristor (the dimensions of the current is really dependant on the dimensions of the burden and the dimensions of Ea), and so the thyristor is totally excited. This conduction process is completed in a really short time.
- After the thyristor is excited, its conductive state is going to be maintained by the positive feedback effect from the tube itself. Even if the forward voltage from the control electrode disappears, it is actually still inside the conductive state. Therefore, the function of the control electrode is simply to trigger the thyristor to transform on. After the thyristor is excited, the control electrode loses its function.
- The only way to shut off the turned-on thyristor is to lessen the anode current that it is insufficient to maintain the positive feedback process. The way to lessen the anode current is to cut off the forward power supply Ea or reverse the bond of Ea. The minimum anode current necessary to keep your thyristor inside the conducting state is referred to as the holding current from the thyristor. Therefore, strictly speaking, provided that the anode current is less than the holding current, the thyristor can be switched off.
What exactly is the distinction between a transistor along with a thyristor?
Structure
Transistors usually include a PNP or NPN structure composed of three semiconductor materials.
The thyristor consists of four PNPN structures of semiconductor materials, including anode, cathode, and control electrode.
Working conditions:
The work of any transistor relies on electrical signals to control its opening and closing, allowing fast switching operations.
The thyristor needs a forward voltage along with a trigger current on the gate to transform on or off.
Application areas
Transistors are widely used in amplification, switches, oscillators, along with other facets of electronic circuits.
Thyristors are mainly found in electronic circuits such as controlled rectification, AC voltage regulation, contactless electronic switches, inverters, and frequency conversions.
Means of working
The transistor controls the collector current by holding the base current to attain current amplification.
The thyristor is excited or off by manipulating the trigger voltage from the control electrode to realize the switching function.
Circuit parameters
The circuit parameters of thyristors are related to stability and reliability and in most cases have higher turn-off voltage and larger on-current.
To summarize, although transistors and thyristors may be used in similar applications in some cases, because of their different structures and working principles, they have noticeable differences in performance and use occasions.
Application scope of thyristor
- In power electronic equipment, thyristors may be used in frequency converters, motor controllers, welding machines, power supplies, etc.
- Inside the lighting field, thyristors may be used in dimmers and light control devices.
- In induction cookers and electric water heaters, thyristors can be used to control the current flow towards the heating element.
- In electric vehicles, transistors may be used in motor controllers.
Supplier
PDDN Photoelectron Technology Co., Ltd is a wonderful thyristor supplier. It really is one from the leading enterprises in the Home Accessory & Solar Power System, that is fully involved in the growth and development of power industry, intelligent operation and maintenance handling of power plants, solar power and related solar products manufacturing.
It accepts payment via Bank Card, T/T, West Union and Paypal. PDDN will ship the goods to customers overseas through FedEx, DHL, by air, or by sea. If you are searching for high-quality thyristor, please feel free to contact us and send an inquiry.
